In part 1 we examined the importance of what load management is and how this can impact the likelihood of sustaining a running related injury. Part 2 will examine different aspects of running form and their association with different running injuries.
Running gait and Injury?
If you are a runner reading this you have probably as some point had a running injury. Luckily most injuries can be settled with a brief period of rest and possibly some exercises to improve the strength and condition of our musculoskeletal system.
Frustratingly, however, some injuries just seem to keep recurring no matter what the runner does. Strength training alone may not be enough to sort out the problem. If a runner continues to place repeated stress in a certain area due to the way he or she runs the injury will keep re-curring. Willy and Davis (2011) demonstrated that although a hip strengthening programme improved strength and squat mechanics it did not change running mechanics. On the other hand, Noehren (2010), demonstrated that gait retraining on a treadmill using visual and verbal feedback in individuals with patello-femoral (knee cap) pain resulted in significant improvement of both hip mechanics and a reduction in pain when running.
Common Running Faults and Injury
Initial Foot Strike:
Initial foot strike is where we land when we first touch the ground. Some of the more common patterns we see are as follows:

Over-striding: This is landing with the foot too far in front of the body. Tight or overactive hip flexors (muscles are the front of the body), weak gluteals muscles (buttocks), poor trunk control, and slow running cadence (how many steps you take per minute) can lead to over-striding. It can cause a number of running related injuries. In particular knee injuries such as patello-femoral pain (PFP) or Ileotibial band syndrome (ITBS) are commonly associated with this pattern.
Tip
- Count how many strides you are doing in a minute. The gold standard in research is 180 strides per minute but we are all individuals so this may not suit everyone. If your cadence is less than 170 strides aim to increase the total by 5-7%. Do not attempt this for the whole of your next run. Introduce gradually over a period of sessions.
- Runners who over stride often are quite bouncy so think about running as if their was a ceiling just an inch above your head to encourage you to go forward and not up and down.
Landing with a Straight Knee. This is often associated with over-striding and weakness of the quadriceps muscles. It can be linked to injuries such as hamstring, PFP, achilles tendinopathy, and ITBS.

Tip
- Increasing cadence may help with this but introducing some strength and conditioning to improve the strength of the quadriceps and gluteal muscles.
Landing with too much Knee Bend. Normal knee bend is around 10-15 degrees on landing. Greater than this may be a cause of weak quadriceps, hamstrings and calf. It is linked with injuries of the knee including PFP and ITBs.
Tip
- Check your run cadence and increase strength in quadriceps, gluteals and hamstrings.
Mid Stance Faults:
Mid Stance occurs after the initial strike when the foot is flat on the ground. Some of the common fault we can see are:
Reduced Knee Bend. Running with a stiff knee can be associated with quadriceps weakness and stiffness at the ankle joint. It is linked with injuries of the patella tendon, PFP, achilles tendinopathy and plantar-fasciopathy (pain in the heel).
Tip
- Increasing cadence, aim of reduce the heavy sound when you run. Again adding in quadriceps and gluteal strengthening to reduce the impact forces around the knee.
Too Much Ankle and Knee Bend. The angle between the foot and the shin bone shouldn’t increase much beyond 20 degrees. This pattern is often associated with weakness in the calf muscles, quadriceps, gluteals and hamstrings. It is also a pattern commonly seen with over-striding. Increased stress placed upon the tendon and fascia in the calf and foot can lead to achilles tendinopathy and plantar fasciopathy.

Tip
- Strengthen in particular the calf muscles and when running think about picking up the foot as quickly as you can off the ground. Listen to the sound when you run and if you sound really heavy then aim to run lightly.
- Think of a forward impulse and not up and down.
Propulsion:
Propulsion occurs after mid-stance as we push off in the gait cycle.
Lack of Hip Extension: As you push off the hip should extended to about 10-15 degrees. Tight muscles around the front of the hip can restrict this. Weakness in the gluteals and calf muscles will also reduce your ability to propel yourself forward. Pushing harder with the calf can cause fatigue of the muscle and over use injuries such as achilles tendinopathy. Restriction in the hip flexors may lead to an increase in patello-femoral pain or hip impingement pain.
Tip
- Improve the mobility of the muscles at the front of the thigh to allow sufficient movement for the hip to extend.
- Strengthen the gluteals into extension with exercises such as the bridge and the step up.
Looking From Behind:
Pelvic Drop: Pelvic drop is seen when we land and the opposite side of the pelvis drops down. This is associated with weak gluteals and trunk muscles on the landing side but may also be related to foot pronation where the foot falls inwards and a stiff ankle joint. The research has shown that gluteal weakness is linked with knee injuries such as PFP and ITBS.

Left Side: Less pelvic drop following gait retraining and muscle strength training.
Tip
- Focus on cadence – see above
- Imagine headlamps on the front of the pelvis and imagine keeping them shining parallel to each other
- Strengthen the gluteal complex.
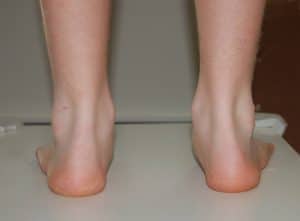
Foot Pronation: This is where you will see the foot rolling inwards as the foot contacts and lands. It is a normal process of running gait but over-pronation is often blamed as a reason for a number of running injuries. The research is not conclusive as to the true effects of over-pronation and injury. However, rolling inwards too quickly or prolonged over-pronatation may lead to injury. Common injuries associated with this pattern are plantar fasicopathy, achilles tendinopathy, PFP, to name but a few.
Tip
- Ensure adequate foot and calf muscles strength
- Improve gluteal strength
- Seek advice as to whether an orthotic may help
Stop Running in Pain and Click Book Now to Receive 10% off until The End of December 2017. Quote “Run10” when booking.
Summary
Video Analysis: This will identify any faults that may be contributing to the injury. A trained professional in running gait analysis will establish if your running gait can be altered and facilitate these changes with simple cues and drills. They will also determine any areas requiring strength or increased flexibility.
Count your cadence: Studies have shown that reducing over-stride and increasing step rate will lead to an overall reduction in force going through the body. Simply taking smaller quicker steps can help to reduce this over striding pattern.
Make gradual Changes: Any changes you make to your running style needs to be done gradually to allow the bodies tissues time to adapt.
Improve your overall strength: Running retraining is not enough on it’s own to make substantial improvements and reduction in injury in the long term. Many running patterns are associated with weak areas in our musculoskeletal system. Introducing strength and conditioning into your programme will not only reduce the likelihood of running related injuries but also improve your performance. Beattie et al. (2014) in systematic review assessing strength and conditioning on performance of endurance runners demonstrated improved time trial performance at 3km and 5km, improved VO2 max, improved running economy and improved muscle power.
References:
Willy, R.W., Davis, I.S., 2001. The effect of a hip strengthening program on mechanics during running and during a single leg squat. J Orthop Sports Phys Ther 41, 625-632.
Noehren, B., Scholz, J., Davis I., (2011) The effect of real-time gait retraining on hip kinematics, pain and function in subjects with patellofemoral pain syndrome. British Journal of Sports Medicine 45 (9) 691-696.
Beattie, K., Kenny, I.C., Lyons, M., Carson, B.P. (2014) The effect of strength training on performance in endurance athletes. Sports Medicine 44 (6) 845-865.

